In June 2019, I underwent pelvic vein embolization at The Whiteley Clinic to treat pelvic congestion syndrome — a culprit in pelvic pain for up to 30% of women and men. Here is my experience, including why I chose The Whiteley Clinic for the best diagnostic imaging and pelvic vein embolization.
Click here to schedule a PCS Peer Support Consult with me!

On June 8, 2019, I had 13 platinum coils placed in my pelvic veins by Dr. David Beckett at The Whiteley Clinic to stop pelvic venous reflux, also know as pelvic congestion syndrome.
If you’ve never visited my site before or if you’re looking for more info about pelvic congestion syndrome, check out my other PCS posts:
- So You’ve Been Diagnosed with Pelvic Congestion Syndrome? Here’s What You Need to Know
- 20 Ways to Relieve PCS Pain
- 11 Questions to Ask Your Doctor Before Treating Pelvic Congestion Syndrome
- How to Find a Qualified Interventional Radiologist to Treat PCS (video with Dr. David Beckett)
I am also available to offer help via PCS Peer Support. Click here to email me and learn more!
Before the surgery, I had spent several bed-ridden months in pain, having daily panic attacks, and feeling more lost than I ever have. Yet, there were pockets of time that I used to research and learn everything about pelvic congestion syndrome that I could.
By the time I saw the interventional radiologist in a nearby city, I had read published papers, journal articles, and online posts about pelvic congestion syndrome. I found a lot of conflicting information, but still showed up to my IR appointment with a notebook full of studies and questions.
I asked questions, brought up topics, and referenced studies about PCS. Honestly, I felt like the most educated person in the room.
When this interventional radiologist told me I appeared to have Nutcracker Syndrome and that he did 3 or 4 pelvic vein embolizations per year, I made up my mind: he would NOT be placing anything inside my body!
I had waited 3 months to see this guy. That was 3 months of research, hoping for answers, and most importantly, hoping for a path to treatment and healing.
But, I left disappointed and basically feeling like I was starting back at square one. So, back to the computer I went.
By this point, I wasn’t sure what else I could find to help myself with PCS. I had already done so much extensive and exhausting research!
I needed a specialist, but where would I go? Even The Mayo Clinic and Johns-Hopkins didn’t have great research or knowledge of PCS.
One last time, I went back to Google and saw an article from The Whiteley Clinic that I had scrolled past several times without clicking.

Me and Dr./Professor Mark Whiteley
How I Found The Whiteley Clinic
Why hadn’t I clicked it before?
Because I saw that it was in the United Kingdom. Up until that point, I hadn’t even entertained the possibility of reading information from overseas. Living in the United States, one often believes that the best medical care is available right here.
Unfortunately, this is not the case with pelvic congestion syndrome. American OBGYNs, ultrasound technicians, interventional radiologists, phlebologists, and vascular surgeons are way behind when it comes to the best diagnostic procedures and treatment for PCS.
I had already spent months in bed. I was on anti-anxiety medications and trying to support my gut health while on these meds. And, I had even attempted suicide and checked myself into in-patient mental healthcare for 5 days.
I had NOTHING to lose.
So, I clicked, read the article, and found contact information on The Whiteley Clinic’s website. I sent an email to the clinic with no expectations whatsoever.
Within 12 hours, Dr. Mark Whiteley himself sent me a reply, part of which you can read below.

Finally! Someone who made sense and actually knew what they were talking about!
Dr. Whiteley and I corresponded a few times over the next several days. Then, we set up a Skype consult.
I also Skyped with leading interventional radiologist Dr. David Beckett who reviewed my CT scans (the only diagnostic imaging I had at this point) and determined that I was a good candidate to fly over for scans and scheduled embolization.

Me and Dr. David Beckett
After chatting with Dr. Beckett, I’d made up my mind. Come hell or high water, I was going to the UK to receive the correct diagnostic imaging and treatment for pelvic congestion syndrome.
The remainder of this post is an explanation of exactly what happened during my time at The Whiteley Clinic, including the special trans-vaginal/trans-abdominal ultrasound, the embolization procedure, my recovery, and the results. I get a lot of emails and comments on the blog with questions, so I’m answering those at the end.
Trans-Vaginal/Trans-Abdominal Ultrasound Using the Holdstock-Harrison Protocol
Contrary to American doctors, pelvic congestion syndrome should not be diagnosed using CT scan, MRI, laparoscopy, or IVUS. These modalities can be used to rule out other causes of pelvic pain, such as endometriosis, uterine fibroids, or ovarian cysts, but they are not the best tools for properly diagnosing PCS.
The correct diagnostic imaging for PCS is a trans-vaginal/trans-abdominal doppler ultrasound using the Holdstock-Harrison and Holdstock-White Protocols.
Currently, Dr. Whiteley nor I know of any vascular clinics or doctors in the United States who use this specialized technique to properly and adequately diagnose pelvic venous reflux. Watch my interview with Professor Whiteley to learn why these ultrasound techniques are the gold standard of PCS diagnosis!
Click here to contact me about a PCS Peer Support Consult.

At The Whiteley Clinic’s Guildford location in Surrey, I met with Angie White, a sonographer who’s been studying, writing, and publishing the research about this type of ultrasound.
I felt absolutely at ease with Angie.
Unlike American sonographers, Angie was actually able to talk me through the entire ultrasound — pointing out on the screen where the venous reflux was present.
It was the most thorough ultrasound I’ve ever had! In addition to looking for refluxing veins, Angie checked my liver and gallbladder, ovaries and uterus, bladder, and kidneys.

When the Holdstock-Harrison Protocol was used (tipping me backwards on the table), my left renal vein opened up completely — indicating no actual Nutcracker Syndrome! (This is what Dr. Whiteley and Angie have termed “pseudo-Nutcracker” and it is very common, but true Nutcracker Syndrome is very rare.)
The verdict?
Severe venous reflux in the left ovarian vein and left and right iliac veins.

Pelvic Vein Embolization at The Whiteley Clinic
Pelvic vein embolization was my next step. So, 2 days after the sonogram with Angie, I went to the London clinic.
Pelvic vein embolization at The Whiteley Clinic is very different from this procedure in the United States.
In the US, embolization is typically done in a hospital as outpatient surgery. It requires a couple of hours, sedation or light anesthesia, and a recovery time of a few hours.
However, at The Whiteley Clinic, pelvic vein embolization is a simple, quick, walk in/walk out procedure.
I was treated like royalty the entire time I was there. All of the nurses were compassionate, understanding, and patient.
I had a fair amount of anxiety during the procedure, and they were all so kind. Even Dr. Beckett, my surgeon, wasn’t annoyed or hasty during the procedure despite my shaking!
I had 13 platinum coils placed in my left and right obturator veins, left and right pudendal veins, and left ovarian vein in less than 45 minutes.
Immediately after the procedure, I was escorted to a recovery area where Dr. Beckett explained the entire embolization. Here’s a video of his post-op explanation:
Pelvic Vein Embolization Recovery & Follow-Up
Since I hadn’t eaten that morning, my blood sugar was quite low. The only snacks The Whiteley Clinic had were tea biscuits made with gluten and dairy, so they actually went around the corner to a Pret coffee shop and brought back a gluten-free and vegan avocado toast for me!
After I ate my toast and drank a cup of tea, I was ready to leave.
My husband and I spent the afternoon walking around Borough Market together. It was one of my favorite places in London!
When we returned to our flat that evening, I had started feeling very tired. I ran a bath and soaked in the tub for about an hour, and it felt so good!
Crazy enough, my period came that evening, too. It must’ve been the stress or all that was going on in my pelvis, because my cycle came 5 days early.
Three days after surgery, I returned to the clinic for another sonogram with Angie. This follow-up ultrasound checked the coils and confirmed that the embolization stopped all reflux. I was all clear — no remaining pelvic congestion!
Two days later, we boarded our flight home!
Now, I’ll answer the most frequently asked questions I get in emails and comments.

What was the sonogram like?
It was thorough, long, and extensive!
Seriously, 90 minutes, I think?
For the transabdominal part, I started by sitting sitting upright. Then, I was laid back. And then, tilted backwards to check for Nutcracker Syndrome.

The transvaginal part was just as in-depth. It wasn’t uncomfortable at all. At times, I had to bear down or contract my pelvic floor muscles.
Angie explained every, single thing on the screen throughout the entire process.
Did you do anything to prepare for the embolization?
Yes! I knew that I needed to prepare mentally, physically, and emotionally for this procedure in order to have the best possible result.
Mentally, I spent time in meditation. I envisioned having the procedure and visualized my future self free of PCS symptoms.
Emotionally, I felt I needed to thank my broken veins for their years of service. I thanked my veins for doing their best to function for over 35 years. I also apologized for all the pain and dysfunction they’d experienced. And, I said goodbye to them. It was a special moment with my body.
Physically, I started preparing for surgery about 2 months before the procedure. I went to pelvic floor physical therapy, which actually helped the symptoms of PCS! I knew that restoring blood flow, movement, and reducing inflammation in my pelvis was important, and PT was instrumental in that.
Knowing that the coils would cause an inflammatory response, I wanted to reduce all external sources of inflammation.
Diet: Gluten-free, dairy-free, soy-free, sugar-free, legume-free, caffeine-free. Lots of raw greens and sprouts. Ginger and turmeric tea.
Supplements I was either already taking or started 2 months before surgery and continued taking for 12 weeks after:

Liver support: N-Acetyl Cysteine, methylated B vitamins, Aquatic Greens, and Perfect Liver Detox. (Contrast dye is used during embolization, so I wanted my liver to be able to process and eliminate it quickly and efficiently.) Save 10% on Perfect Liver Detox and Aquatic Greens with my discount code ALLTHETHINGS.
Anti-Inflammatory: Turmeric & Piperine Complex
Magnesium glycinate & magnesium citrate (Save 10% on mag citrate with my discount code ALLTHETHINGS.)
Vitamin C for adrenal support (Adrenals are heavily taxed after surgery of any kind. It’s important to support them!)
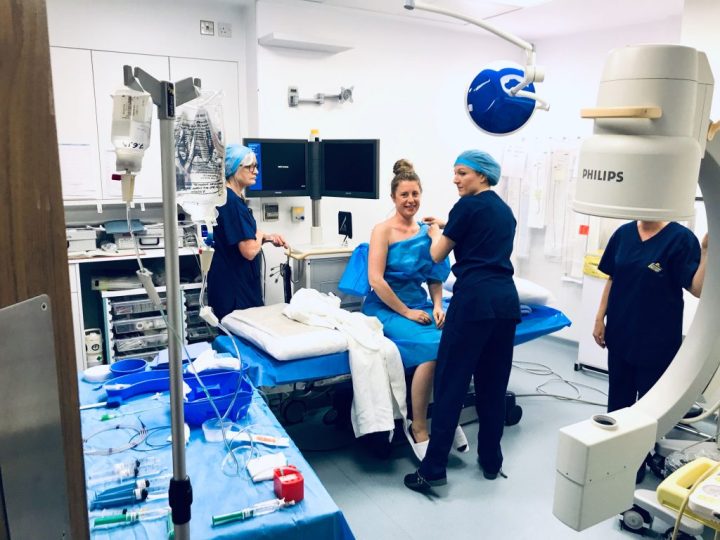
Was it scary to be fully awake for the embolization? Did you feel any pain?
Yes, it was a little scary to be awake.
It was a full operating room experience. Everyone was wearing scrubs, it was very bright, and we were surrounded by equipment. However, I’m grateful that I was awake and can tell the whole experience in full detail.
Dr. Beckett allowed my husband to come into the operating room to hold my hand and help me relax. Having him there calmed me down and got me through the last half of the surgery.
Yes, I did feel some pain. Though, to be fair, my nervous system was fully ON, so I likely felt pain that might’ve been more like pressure or discomfort had my nervous system not been so revved up.
How much did the sonogram and embolization cost?
We paid just under $9,000US for the sonogram and embolization with 13 coils.
The Whiteley Clinic lists pricing on their website. The price listed is the base price for pelvic vein embolization. If you need more or fewer veins embolized, which requires more or less coils, the price goes up or down accordingly.
We don’t have insurance, so I was going to pay out of pocket no matter what. We asked for a price quote from the American interventional radiologist, and it was $63,000 for ONE vein! One vein!
I got more complete treatment for less $9,000 at The Whiteley Clinic, and it was 100% worth it!
Add flights (about $3,000), Air BnB ($1500), and meals (9 days for 2 people = >/< $400) and we were all in at around $14,000.

The Whiteley Clinic’s Guildford location
Can you feel the coils?
Not at all.
The coils are thinner than really small guitar strings and move with my body. I am a highly sensitive person and feel pretty much everything that’s going on in my body, but I do not feel these coils at all.
It is safe for me to go through airport security and to have an MRI with them, too.
What was the immediate recovery like?
Immediately after, I felt great — like normal. We checked the pedometer on our phone when we got back to our flat after walking around Borough Market, and I had walked over 5 miles post-surgery!
That evening, I began running a low-grade fever and having aches and chills. It felt very flu-like, but like a mild flu and definitely no vomiting or nausea.
During our consult at the Guildford clinic, Dr. Whiteley prepared me for possible flu-like symptoms after surgery. The severity and duration of symptoms varies from person to person.
I took a couple of low doses of ibuprofen because I wasn’t sleeping due to the discomfort. Although I avoid medications like this, I was thankful I had it.
When Dr. Whiteley called to check on me the next day, he reassured me that the aches, fever, and chills was my body’s natural inflammatory response, which is the first step in the healing process.
Sure enough, in less than 48 hours, I was feeling much better. On the third day, after my follow-up sonogram, my husband and I walked around Hyde Park, went to the Tower of London, and walked across London Bridge! 7 miles that day! I was definitely slower than usual, but not in pain and not sore.
The plane ride home was as good as can be expected for a 9-hour plane ride. Thankfully, we were on an emergency exit row, so I took advantage of the space to walk around, stretch, and even did some light yoga on the plane!

Did you have any more symptoms of pelvic congestion syndrome after the pelvic vein embolization at The Whiteley Clinic?
Nope! I could tell that the embolization was a success when I walked out of the clinic.
The left-side pain, pelvic pain, and labia pain had gone away.
As soon as we returned home, I was back to doing all the things I love. I spent a beautiful summer gardening, hiking, swimming, and going for daily walks — things I couldn’t do without extreme pain just a few months earlier!
My long-term recovery wasn’t totally pain-free, though. In fact, I’ve exchanged a few emails with Dr. Whiteley in the months following embolization when I felt an odd pain or sensation that I thought to be a PCS recurrence.
But, I have proof that the reflux is gone and the likelihood of other veins refluxing after this procedure is very, very slight (like a 3-4% chance).
Here’s the truth: pelvic vein embolization permanently altered my anatomy. Although I have no symptoms of PCS (and I’m so thankful for that!), I still have 13 metal coils in my pelvis that aren’t supposed to be there.
Just because the PCS is gone doesn’t mean all pelvic pain magically disappeared.
Since the embolization, I have worked closely with my pelvic floor physical therapist. She has greatly assisted my long-term recovery with techniques such as myofascial release, muscle release, lymphatic drainage, restoring blood flow and symmetry to my pelvis, pelvic floor, and low back, and more.
Any minor pain I have now isn’t constant or severe, doesn’t prevent me from doing anything I want to do, and is pretty easy to ignore. It’s also not PCS pain — of that I am sure!
In hindsight, what would you do differently?
The biggest mistake I made was joining Facebook “support” groups for pelvic congestion syndrome.
If you want to feel depressed and hopeless about a PCS diagnosis, head on over to Facebook! It’s dismal, y’all.
I went looking for research and information. Instead, I found a lot of moaning and complaining and misinformation.
I know these women were in a lot of pain — sometimes decades of pain — which is completely unfair and sad.
Many of these women had undergone pelvic vein embolization and felt worse than ever. Even more of them claimed that they had reactions to the coils or the coils poked out of their veins, causing a host of new issues.
Many were advocating hysterectomies as the best course of treatment.
Lots of these women claimed that birth control pills or gabapentin were the answer for treating PCS.
I know all of their stories were and are real, but I also knew that didn’t have to be MY story.
I am grateful that these groups alerted me to issues like compressions (such as May-Thurner Syndrome and Nutcracker Syndrome) and to the material of which the coils are made.
After that, however, I promptly left (and was even kicked out of 1) these groups. I found my own way, and I am grateful that I stuck with the research and didn’t give up on myself.
Because of my stick-to-it-ness, I found the best doctors and clinic in the world for the condition I had!

The Whiteley Clinic in London
What advice would you give to someone with PCS?
Just get your sonogram and pelvic vein embolization at The Whiteley Clinic. I’m serious!
You deserve the best, and Dr. Whiteley, Angie, and Dr. Beckett are the BEST.
It’s not extreme at all to go across an ocean for the best medical care. Our health is our most valuable resource, after all!
American doctors really are not qualified to be diagnosing and treating PCS, in my opinion. I hope that more American doctors are willing to study and learn the diagnostic techniques and procedures that The Whiteley Clinic have developed.
Until that happens, please save yourself a lot of trouble (and potentially not getting relief) and just go see Dr. Whiteley.
Can’t afford it?
Well, we couldn’t either! A special friend started a fundraiser for us, and then my grandfather sent us a large sum of money. So, we didn’t pay out of pocket for this, and you may not have to either.
Don’t be ashamed to ask for help. People love you and want to support you and help you! Let them give you that gift and show you love in that way with no shame!
Second, work with a pelvic floor physical therapist before and after embolization. I truly believe I experienced quicker healing because I of pelvic floor PT. Read about my diagnosis, treatment, and recovery from pelvic floor dysfunction.
Third, learn to advocate for yourself! We can’t 100% trust anyone when it comes to our health because no one has to live in our bodies but us.
I am SO grateful that I had those months in bed because I had time to learn and research what I needed to know to make informed choices and advocate for myself and my health. So many women just let doctors do things to them, often with less than optimal results.
I am not that woman. You shouldn’t be either.
With a whole world of resources at our fingertips (Internet), we have no reason not to educate ourselves — and I don’t mean joining Facebook support groups (which was the WORST thing I did).
Believe that you deserve the best, that you have a reason to hope, and that help is available if you know where to find it!
Pin it!

